Case Report

Anterior Neck Giant Atypical Lipoma: A Case Report and Review of Literature
1Ram Niwas Meena,1SK Tiwary2Amit Kumar Yadav, 2Vipul Srivastava, 2 Akshay BR, 2Sweety Kumari,3 Rahul Khanna
- 1MS, Associate Professor, Department of General Surgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi, UP, India.
- 2MBBS, Resident, Department of General Surgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi, UP, India.
- 3MS, Professor, Department of General Surgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi, UP, India.
- Submitted:Saturday, April 25, 2020
- Accepted: : Monday, May 18, 2020
- Published:Thursday, May 28, 2020
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/4.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited
Abstract
Background
Lipomas are benign mesenchymal tumour. They constitute 5% of all benign tumors of body and can be found anywhere in the body, 13% of lipomas are seen in head and neck region, Anterior neck lipoma is a rare one specially of hanging like bell is extremely rare. A lipoma is considered to be of giant when it’s size greater than 10 cm in length (in any dimension) or weighs over 1000 gm.
Case report
We are reporting a case of 50 year old male who presented with a huge swelling in the anterior neck region for last 20 year and sudden increase in size from 6 month. FNAC and sonography confirmed the diagnosis of lipoma. Enucleation of lipoma with redunded skin from neck was done and followed up for 1 year without any complication.
Conclusion
Giant pediculated lipoma of the anterior neck is extremely rare. Surgical management of this tumor is challenging and should be performed by an experienced surgeon due to the need for meticulous dissection with respect to the underlying blood vessels and nerve.
Key words
Giant pediculated lipoma, anterior neck lipoma, mesenchymal tumour
Introduction
Lipomas are the most common benign mesenchymal neoplasm of adulthood and are usually subcutaneous but may develop in other places, e.g. intermuscular, subfascial, parosteal, subserous, submucous, intra-articular, subsynovial, subendocardium, subepicardiac, myocardium, subdural or extradural. They are actually a cluster of fat cells which become overactive. This is the commonest tumor of subcutaneous tissue. They are skin colored lesions, firm and somewhat lobulated on palpation. Common sites of lipoma are back, arms, shoulder, anterior chest wall, breasts, thighs, abdominal wall, legs, forehead and face [1]. In head and neck region, where only 13% of lipomas are seen, posterior cervical space is the commonest site [2]. Anterior neck lipoma is a rare location for lipoma [3] and anterior neck lipoma with hanging in neck is very rare.
Lipomas infrequently occur in the head and neck. Giant lipomas are defined by Sanchez et al as lesions with size of at least 10 cm in one dimension or weighing a minimum of 1,000 gm [4]. A large neck mass (>10 cm) with a rapid growth rate should raise concerns about a possible malignancy [4]. Although the diagnosis is mostly clinical, imaging tools are useful to confirm the adipose nature of the lesion and to define its anatomic border. Surgical excision of a lipoma is often used as the definitive treatment.
Most of head and neck lipomas are superficial and present in the posterior region of the neck. On the other hand, lipomas in the anterior neck are uncommon. Only very few cases have been reported in the literature [3, 5-10]. We report a case of atypical giant lipoma of the anterior neck.
Case Report
A 50 year old male presented with swelling in the anterior part of neck for last 20 years. The swelling was gradually progressive; with rapid increase in size over last 6 months. No history of change in voice, breathlessness, dysphagia, sleep disturbance and no history of comorbid conditions was present.
On examination patient’s vitals was normal, swelling was present on anterior aspect of neck and was freely mobile in all directions and hanging from neck to abdomen it was soft in consistency. Venous engorgement was present over swelling and two ulcers present on inner expect of swelling, ulcers has everted edge and irregular margin (Fig 1). X-ray of neck and chest demonstrated a soft tissue mask from neck to chest. Bilateral lateral lung field were clear and there was no compression of trachea (Fig 2). Blood investigation within normal limits and FNAC from swelling was suggestive of benign lipoma. The lipoma was surgically excised under general anaesthesia by elliptical incision on the neck and raising flaps (Fig 3), redunded skin was excised, haemostasis was archived and a drain placed and would was closed. Weight of lipoma was 6.4 kg with diameter of 21 x 12 cm size. The histopathology report confirmed the diagnosis of a benign lipoma. Post-operative period was uneventful with no recurrence at 6 months follow-up.
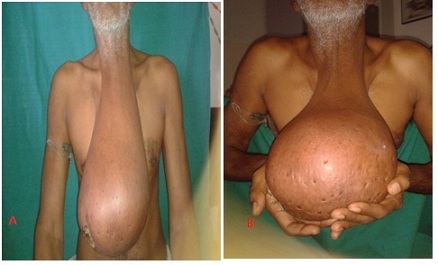

Figure 1a& b: Preoperative photo of patient with giant hanging lipoma in anterior aspect of neck

Figure 2a b: X-ray of neck (AP & Lateral view): showing large hanging soft tissue shadow of swelling in anterior aspect of neck upto thorax

Figure 3: Resected speciemen of Lipoma weight 6.4 kg and size 21x12 cm.
Discussion:
Lipoma is one of the commonest benign mesenchymal tumours in the body composed of mature adipose cells. It is found in almost all the organs of the body where normally fat exists that is why it is also known as ubiquitous tumour or universal tumour [11]. Lipoma is seen in all age group though mostly seen in fifth and sixth decade [12] as in our case it was in fifth decade of life, it constitutes five percent of all benign tumors of body and can be found anywhere in the body [13]. Lipoma in head and neck region is not commonly amongst the head and neck lipomas, commonest location is posterior neck [2]. Anterior neck is a rare location for head and neck lipoma [3]. Lipoma of anterior neck with hanging like bell on thorax is very rare.
Lipomas are slow growing, painless, mobile, non-fluctuant, soft masses&are generally well encapsulated. Lipomas can be singular or multiple and are typically asymptomatic unless they compress neurovascular structures. Beside frequent aesthetic consequences, lipomas can also exert pressure on surrounding tissues and structures. A long standing lipoma may undergo myxomatous degeneration, saponification, calcification, infection, ulceration due to repeated trauma, as our case has two ulcers on inner aspect of lipoma and malignant change. Rarely malignant transformation of lipoma into liposarcoma has been described [14].
Histologically lipomas are composed of mature adipose tissue, and several subtypes occur when other mesenchymal elements are present [15], for example fibrous tissue, nervous tissue or vascular tissue. According to WHO classification of soft tumours these can be classified into nine groups, including lipoma, lipomatosis, lipoblastoma, angiolipoma, myolipoma of soft tissues, chondroid lipoma, spindle cell lipoma, and finally hibernoma and pleomorphic lipoma [16]. Most common subtype is conventional lipoma which is well encapsulated mass of mature adipocytes and varies considerably in size. All subtypes are painless except angiolipoma. Hibernomas are benign, uncommon tumors presumably arising from brown fat that may occur in the back, hips, or neck in adults and infants& has a slightly greater tendency to bleed during excision and to recur if intralesional excision is performed.
The characteristic sonographic appearance of head and neck lipomas is that of an elliptical mass parallel to the skin surface that is mostly hyperechoic relative to adjacent muscle and that contains linear echogenic lines at right angles to the ultrasound beam [17].
Computed tomography is modality of choice to confirm lipoma. Lipomas appear as homogenous low density areas with a CT value of -50 to -150 HU with no contrast enhancement [18]. A significant soft tissue element or heterogeneity of attenuation within a fatty lesion raises the possibility of liposarcoma.
In MRI, lipomas have well defined margins with a uniform signal intensity of fat on all sequences. Some lipomas may also have internal septa, an appearance mimicking a well differentiated liposarcoma (termed atypical lipoma). Margin of lipoma is clearly defined as “black rim”, distinguishing them from surrounding fat [19]. Calcification is rare & forms centrally within an area of ischaemic necrosis but more commonly it’s a feature of a liposarcoma.
Surgical excision of lipoma is the definitive treatment. Surgery is reserved for patients coming for cosmesis (most common indication) and pressure effects & to rule out malignancy. Surgical intervention of giant lipoma of anterior neck is challenging because of proximity to the great vessels, vagus and spinal accessory nerves. Complete surgical excision with the capsule is advocated to prevent local recurrence.
Other modalities of treatment have been reported, like liposuction [20] and steroid injections. Liposuction is sometimes preferred as there is less scarring [20] following the procedure but there is higher chance of recurrence compared to excision if residual tumour or capsule, remains after the procedure. For smaller lipomas steroid injections may also be used, but several injections are required and the overlying skin may be depigmented.
Conclusion:
Giant pediculated lipoma of the anterior neck is extremely rare. Surgical management of this tumor is challenging and should be performed by an experienced surgeon due to the need for meticulous dissection with respect to the underlying blood vessels and nerve. Giant lipomas in an elderly patient may mimic malignancy. Therefore, surgeons must be aware of it. Surgical excision is the treatment of choice.
References:
[1]. Rapidis AD. Lipoma of the oral cavity. Int J Oral Surg. 1982; 11:30-5.[PubMed]
[2]. Barnes L. tumors & tumor like lesions of the head & neck: In: Barnes L, ed. surgical pathology of the head & neck. New York, NY:Dekker; 1985: 747-758.
[3]. Medina CR, Schneider S, Mitra A, Spears J and Mitra A. Giant submental lipoma: Case report and review of the literature. Can J Plast Surg 2007; 15(4):219-222.[Pubmed] [PMC Full text]
[4]. Sanchez MR, Golomb FM, Moy JA, Potozkin JR. Giant lipoma: Case report and review of the literature. J Am Acad Dermatol. 1993; 28:266.[Pubmed]
[5]. Moumoulidis I, Durvasula P, Jani P. Well-circumscribed intramuscular lipoma of the sternocleidomastoid muscle. Auris Nasus Larynx. 2004; 31: 283-285.[Pubmed]
[6]. El-Monem MHA, Gaafar AH, Magdy EA. Lipomas of the head and neck: presentation variability and diagnostic work-up. J Laryngol Otol. 2006; 120: 47-55.[Pubmed]
[7]. Chatterjee S, Prasad S, Nayak SD, Mahato SP. Anterior Neck Lipoma - A Giant Predicament. Hellenic Journal of Surgery 2015;87: 203-205.
[Full Text]
[8]. Gowri Sankar M, Manu CB, Alexander A. Giant Lipoma Anterior Neck: A case report. Archives of Case Reports 2017; 1: 6-8.[Pubmed]
[Full Text]
[9]. Alshadwi A, Nadershah M, Salama A, Bayoumi A. Giant Deep Neck Lipoma: A Case Report and Review of the Literature. Clin Surg. 2017; 2: 1299.
[Full text]
[10]. Arif KN, Juneja R, Tandon S, Malhotra V, Rathore PK. Giant Lipoma of the Neck: A Case Report. MAMC J Med Sci 2017; 3:92-4.
[Full
text]
[11]. Devis C Jr and Gruhn JG. Giant lipoma of the thigh. Arch Surg 1967; 95:151.[pubmed]
[12]. Salam G. Lipoma excision. Is Fam Physician 2002; 65:901-905. [pubmed]
[13]. Enzinger FM, Weiss SW. Benign lipomatous tumors. In: Enzinger FM, Weiss SW, eds. Soft Tissue Tumors. 2nd edn. St Louis: Mosby; 1988.p.301-45.
[14]. Horne, W.J., Lipoma or Cystoma of the Neck. Proc R Soc Med, 1908. 1(Laryngol Sect): p. 38-39. [Pubmed] [PMC full text]
[15]. Mentzel T. Cutaneous Lipomatous Neoplasms. Semi Diagn Pathol, 2001, 18: 250-7. [Pubmed]
[16]. Edmonds JL, Woodroof JM, Ator GA: Middle-ear lipoma as a cause of otomastoiditis. J Laryngol Otol 1997, 111(12):1162-1165. [PuBmed]
[17]. Murphey MD, Carroll JF, Flemming DJ, Pope TL, Gannon FH, Kransdorf MJ. From the archives of the AFIP: Benign musculoskeletal lipomatous lesions. Radiographics 2004; 24:1433 66. [pubMed]
[18]. Ahuja AT, King AD, Kew J, King W, Metreweli C. Head and neck lipomas: sonographic appearance. AJNR Am J Neuroradiol 1998; 19:505–508[Pubmed]
[19]. Chikui T, Yonetsu K, Yoshiura K, Miwa K, Kanda S, Ozeki S, et al. Imaging findings of lipomas in the orofacial region with CT, US, and MRI. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 1997;84:88-95.[PubMed]
[20]. Calhoun KH, Bradfield JJ, Thompson C. Liposuction-assisted excision of cervicofacial lipomas. Otolaryngol Head Neck Surg 1995; 113:401-3. [pubMed]

