Research

Clinical Implications of Delay in the Diagnosis and Treatment of Early Stage Breast Cancer
1Dennis L Citrin, 1Sara J Mortensen, 1Shelly K Smekens, 1Christina M Shannon, 2James F Grutsch
1 Cancer Treatment Centers of America at Midwestern Regional Medical Center, Zion, IL, USA
2 University of Illinois at Chicago, Chicago, IL, USA
Submitted Thursday, September 05, 2013Accepted Thursday, October 17, 2013Published Friday, October 18, 2013
This is an Open Access article distributed under the terms of the Creative Commons Attribution License (http://creativecommons.org/licenses/by/3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
Introduction
We reviewed the incidence and clinical implication of primary treatment delay in a population of newly diagnosed breast cancer patients.
Methods
The original medical record of 591 patients referred to Cancer Treatment Centers of America at Midwestern Regional Medical Center (CTCA/MRMC) with recurrent breast cancer was reviewed and data stored electronically to be analyzed. Approval from our Institutional Review Board (IRB) was not required as this was a retrospective record review with no direct patient contact and no specific patient information or identification was published.
Results
In 95 patients there was a delay of at least six months between the first symptoms of breast cancer and the start of treatment. All but one of the 95 patients presented with a palpable mass. Median delay for the entire group was 18 months. The cause of the delay in starting treatment was; physician error (27/591), patient refusal (65/591) and patient inability to obtain medical care (2/591). Length of delay due to physician error was shorter, and delay due to patients declining medical treatment was significantly longer. Those 23 patients who had attempted to control their disease with alternative treatments before coming to Cancer Treatment Centers of America at Midwestern Regional Medical Center (CTCA/MRMC) were more likely to decline our treatment recommendations.
Conclusions
Delay in diagnosis and treatment of patients with early stage breast cancer is still a common event due to physician error, or more commonly patient reluctance to seek treatment. Delay is associated with higher probability of advanced disease.
Introduction
It has been recognized for years that the combination of early diagnosis and effective multi-modality treatment has resulted in significant improvement in the overall cure rate for patients with early breast cancer [1-3]. Despite this fact there remains a group of patients where diagnosis and/or treatment of early breast cancer are delayed. We previously studied 30 patients who refused conventional treatment for breast cancer for a minimum of six months in an attempt to understand the psychological basis for treatment delay and refusal [4]. In that study we described two distinct subsets of patients. Eighteen patients either delayed reporting a clinically suspicious breast lump to their physician, or refused appropriate conventional treatment despite biopsy confirmation of breast cancer (Primary Delayers). An additional twelve patients initially received appropriate treatment for their primary disease, but declined further treatment after their disease recurred (Secondary Delayers). In this paper we describe a study of a larger number of patients who delayed initial treatment for newly diagnosed breast cancer, where we focus on the prevalence and clinical implications of primary treatment delay.
Methods
In the present study we attempted to determine the prevalence of primary delay in our patient population by examining the records of all breast cancer patients seen by Dennis L Citrin, MD (DLC) during a twelve-month period (March 2011 through February 2012). All patients whose history revealed a primary delay of at least six months between first symptom or biopsy, and initial treatment were identified. The clinical records of these patients were reviewed to determine the clinical stage and pathological features of their disease at the time of initial treatment, the cause and length of the delay in initiating treatment, and the clinical significance of the delay. Additionally, the details of any alternative cancer treatment used before conventional treatment were recorded. Approval from our Institutional Review Board (IRB) was not required as this was a retrospective record review. Although, informed consent was obtained from the patient (signed consent 2007; DOD 8/23/2011) whose photo is shown in Figure 1
p a
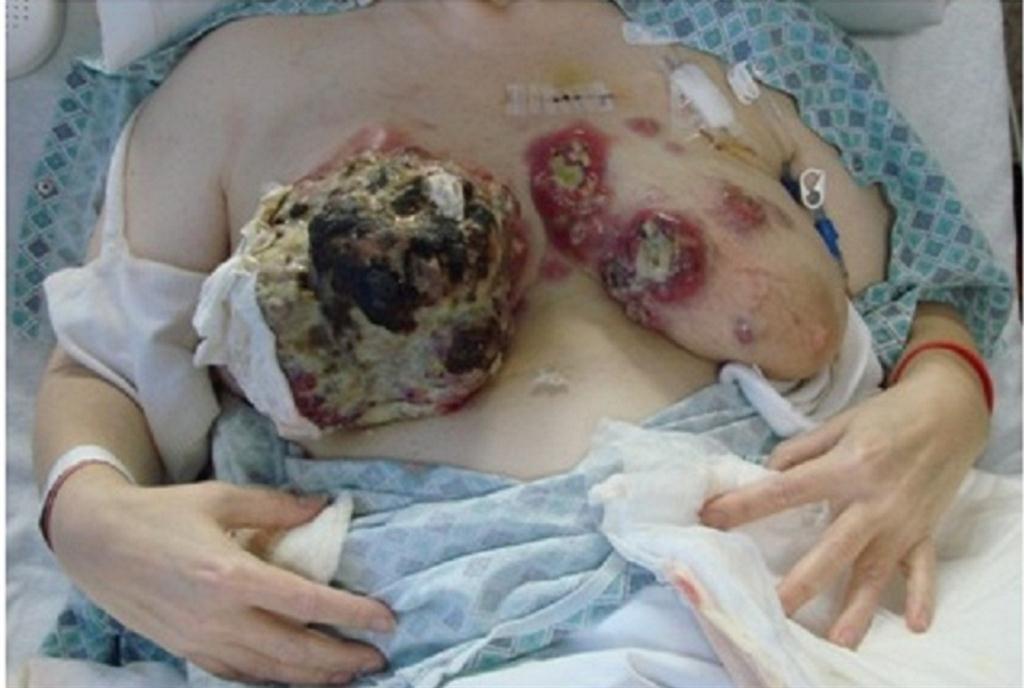
Figure 1: Patient presenting with locally advanced HER2 positive breast cancer after two years of self medication with vegan diet
Results and Discussion
During the twelve-month period March 2011 through February 2012, DLC saw a total of 591 patients with breast cancer at CTCA/MRMC. In 95 of the 591 patients (15.7%) there was a delay of at least six months between the first symptoms of breast cancer, and when the patients started treatment. The median age of those patients who delayed primary treatment was 50 (range 29-73). Seventy-one patients (74.7%) were Caucasian, 19 (20%) were African American, 3 (3.1%) Hispanic and 2 (2.1%) were Asian or Pacific Islander.
Clinically apparent disease at the time of presentation
All but one of the 95 patients initially presented to their primary care physician with a palpable mass (either a lump in the breast or enlarged axillary nodes), the only patient with non-palpable disease was a woman whose initial core needle biopsy of a mammographic abnormality revealed Ductal Carcinoma in Situ (DCIS) only. She refused all treatment, including surgical excision of the area, and came to our institution nine months later, when a repeat biopsy of the same area of mammographic abnormality revealed invasive ductal carcinoma, which was staged as T1aN0M0. When first seen at CTCA/MRMC thirty-two of the 95 patients (33.6%) had locally advanced disease (T3-4 N2-3), and thirteen patients (13.7%) had ulcerated lesions, sometimes to an extreme degree (Figure 1). This example is a middle aged patient that presented with a two year history of a mass in right breast. The patient did not seek medical attention but treated herself with a vegan diet and juicing of fruits and vegetables. She eventually presented with massive tumor involving both breasts. Biopsy confirmed high grade Estrogen Receptor (ER) and Human Epidermal Growth Factor 2 (Her2 neu positive), Progesterone Receptor (PR) negative invasive ductal carcinoma.
Cause of delay in treatment
The cause of delay in initiating treatment was determined in all patients (Table 1).
Table 1: Cause of delay in initiating treatment
|
Physician Error
|
27/591 (4.50%)
|
|
Patient Refusal of Conventional Treatment
|
66/591 (11.10%)
|
|
Patient Inability to Obtain Medical Treatment
|
2/591 (0.003%)
|
|
Total
|
95/591 (15.70%)
|
|
Cause of delay and length of delay
The median delay between first symptom and starting treatment for breast cancer for the entire group was 18 months (range 6-144.) The length of delay was significantly shorter in those patients where delay was due to physician error, and longer in those patients who declined medical treatment while attempting to control their disease with alternative therapies (Kruskal-Wallis p=0.03, Table 2).
Table 2: Cause of treatment delay in relation to length of delay
|
|
Cause of Delay (n)
|
Length of Delay in Months (median and range)
|
|
Physician Error
|
27
|
9 (6-40)
|
|
Patient Delay (no alternative therapies)
|
43
|
12 (6-60)
|
|
Patient Delay (alternative therapies)
|
23
|
18 (6-108)
|
|
Treatment Not Available
|
2
|
6
|
|
Physician error causing delay in diagnosis
Twenty-seven patients complained to their physician of a breast lump, but their physician failed to order a biopsy in a timely fashion. The nature of the physician error is shown in the Table 3.
TAble 3: Physician reassured patient based on clinical examination
|
Physician Reassured Patient Based on Negative Mammogram
|
7
|
|
Ultrasound Read as Simple Cyst
|
8
|
|
Solid Lesion Recognized But No Biopsy Recommended
|
2
|
|
Miscellaneous
|
3*
|
|
Total
|
27
|
|
*One patient presented with a breast mass with ascites and pericardial effusion, initially thought to represent metastatic disease. After a seven-month delay she was eventually diagnosed with a T1cN0M0 breast cancer, her effusions were due to severe hypothyroidism. The second patient presented with an enlarged axillary node, erroneously ascribed to pneumonia, until she was diagnosed with a T2N2M0 breast cancer fifteen months later. A third patient had a history of lymphoma and her T2N1M0 breast cancer was identified on an abnormal Positron Emission Tomography (PET) scan, but ascribed to her lymphoma until the correct diagnosis was made six months later.
Patients induced delay
Sixty-six patients did not seek or accept medical treatment in a timely fashion. Their median age (51) was not different from that of the entire group (50). Forty-eight patients were Caucasian, 15 were African American and 3 were either Hispanic or Asian.
Stage at presentation and length of delay
At the time of presentation to CTCA/MRMC, 39/95 patients (41%) had local disease (T1-2N0-1M0), 32 (34%) had locally advanced disease (T3-4N1-3M0) and 24 (25%) had systemic metastases (M1) (Table 4).
Table 4: Stage at presentation (total in comparison to median delay in months)
|
Local Disease
|
39
|
8 (6-40)
|
|
Locally Advanced Disease
|
32
|
12 (6-108)
|
|
Systemic Metastases
|
24
|
14 (6-80)
|
|
The duration of delay was significantly longer in those patients who presented with systemic metastases (Pearson Chi Square p=0.03).
Details of alternative treatments employed
Of the sixty-six patients who delayed conventional cancer treatment, 23 (35%) reported using some form of alternative treatment. Most tried more than one treatment modality, and described researching alternative treatments on the Internet. The most commonly used modalities were herbs, supplements and vitamins (including intravenous Vitamin C) 25 patients; dietary modification (including juicing) 15 patients, acupuncture and chiropractic manipulation 4 patients; and a variety of other measures which included homeopathy, hydrogen peroxide and ozone, anti-oxidants, mercury detoxification, coffee enemas, Laetrile, shark cartilage, reflexology, colonics, “telephone monitoring,” and topical estrogen or black salve applied to the breast.
All of the 23 patients who used alternative treatments as first therapy for their breast cancer consulted with and received treatment from at least one health care provider, none of whom apparently had formal oncology training.
Patient Compliance with Treatment Recommendations at MRMC
The majority of patient’s 86/95 (90.5%) accepted appropriate conventional treatment at CTCA/MRMC. All but 1 of the 24 patients presenting with systemic metastatic disease fully accepted our treatment recommendations. Nine patients (9.5%) did not accept appropriate treatment per National Comprehensive Cancer Network (NCCN) guidelines. Those patients who had attempted to control their disease with alternative treatments before coming to CTCA/MRMC were more likely to decline our treatment recommendations. The mean delay in the 9 patients who declined our treatment recommendations (34 months) was significantly longer than those who accepted our recommendations (15 months) (Mann-Whitney P = 0.04).
Conclusions
This is a retrospective analysis of a relatively small number of patients. It appears from this study however, that many women with early stage breast cancer are still experiencing a significant delay in obtaining a diagnosis or initiating appropriate treatment.
Clinical significance of delay
Those patients presenting with locally advanced disease (Stage 3) and systemic metastases (Stage 4) had significant longer delay than those presenting with local disease only (Stage 1 and 2). Our findings are consistent with previously published studies, which confirm a poorer prognosis in patients who experienced a delay in diagnosis [5].
Cause of delay in diagnosis
This study confirms that there appears to be two distinct reasons for delay in diagnosis in the present study, physician error and inappropriate patient choices [6].
Physician error
There was a significant delay in the diagnosis of breast cancer in 27 of 591 patients (4.6%) due to physician error. It is troubling that in our patient population nearly 5% of patients were initially reassured by their doctor that they did not have cancer, with little clinical information to support this assumption. This practice continues, despite the well documented inability of clinical examination and a negative mammogram to reliably determine whether a palpable breast mass is benign or malignant [7-14]. It is particularly disappointing that such errors continue to occur despite the development and publication of protocols for the appropriate diagnostic evaluation of women with a palpable lump in the breast [15-16]. If our patient population is representative of the general breast cancer population, a 5% incidence of diagnostic delay due to physician error would indicate that approximately 10,000 women with breast cancer are not being diagnosed in a timely fashion every year in the United States. Our estimates of the prevalence of this problem are very similar to previous reports [14]. The leading cause of physician delay in diagnosis of breast cancer continues to be inappropriate reassurance that a mass is benign without biopsy. Reducing delay in diagnosis due to physician error requires physicians to recognize that they cannot rely on their clinical examination to decide that a mass is benign, and also to recognize the limitations of mammography in this regard. The initial diagnosis of breast cancer is generally not the responsibility of the oncologist, so the appropriate diagnostic evaluation and prompt diagnosis of breast cancer remains an important educational topic for primary care physicians: family doctors, general practitioners and gynecologists [17].
Diagnostic and treatment delay due to patient choice
The second cause of delay is in some ways even more troubling. In our study, more than one in ten women who felt a breast lump that they suspected was cancer either delayed seeing a doctor to confirm the diagnosis or refused appropriate treatment, even in the face of a positive biopsy. At least one third of the women who delayed appropriate treatment attempted to control their disease using one or more of a variety of unproven methods of natural healing. They continued using these “treatments” for eighteen months on average, despite obvious disease progression in many cases. They were frequently assisted in this endeavor by a variety of health care providers, none of who appear to have undergone any formal oncology training. This phenomenon is more problematic than delay caused by physician error, as the length of delay in these patients was significantly longer, and the stage of disease at the time of starting appropriate conventional treatment was more advanced. Additionally, the patients whose belief in alternative medicine caused them to delay seeking conventional treatment were more likely to refuse some or all of the cancer treatment, they were offered when they came to CTCA/MRMC (Table 5).
Table 5: Number of patient's non-compliant with CTCA/MRMC Recommendations
|
Physician Error
|
27
|
2 (7.4%)
|
|
Patient Delay (no alternative therapies)
|
43
|
1 (2.3%)
|
|
Patient Delay (alternative therapies)
|
23
|
6 (26%)
|
|
Medical Care Not Available
|
2
|
0 (0%)
|
|
Table 5 address the reasons why patients choose to decline appropriate medical treatment despite obvious clinical signs of disease. Previous studies have identified a number of psychological and socio-economic factors, which increase the probability of patient delay. These include African-American race, low socio-economic status and single marital status [18-22]. In the present study we did not identify any significant differences in the racial, economic or demographic characteristics of those patients who delayed diagnosis, but this may simply be a reflection of the relatively small patient population we studied. It is however our impression that a more important characteristic of those patients who delayed diagnosis is their belief system. In this study, twenty-three of the sixty-six patients who delayed conventional cancer treatment (35%) reported using some form of alternative treatment before seeking conventional cancer treatment.
This experience, together with a high incidence of non-compliance with adjuvant therapy that we have observed in another study [23], makes it clear that there is a significant sub-set of patients with early stage breast cancer who remain unconvinced of the need for, and the efficacy of conventional breast cancer treatment. One of our purposes in writing this paper is to draw attention to the issue of patient delay in seeking medical help when confronted with the strong possibility or confirmation of the diagnosis of breast cancer. It is our hope that patient advocacy groups will devote more resources to educating women regarding the importance of seeking appropriate treatment in a timely fashion. It is encouraging that, when faced with the reality of advanced breast cancer most of the women who initially declined conventional treatment finally accepted appropriate therapy. Despite what was in some cases a delay in initiating treatment for several years, many patients remain potentially curable. It is clear from the results shown here and in an accompanying study [23] that, despite all of the significant scientific advances in breast cancer treatment of the past decade, patient compliance remains an important determinant of treatment success.
Abbrevations
CTCA/MRMC: Cancer Treatment Centers of America at Midwestern Regional Medical Center
DLC: Dennis L Citrin
DCIS: Ductal Carcinoma in Situ
ER: Estrogen Receptor
Her2 neu positive: Human Epidermal Growth Factor 2
PR: Progesterone Receptor
PET: Positron Emission Tomography
NCCN: National Comprehensive Cancer Network
Competing interests
The authors declare that they have no competing interests.
Authors contributions
DLC was the lead investigator of this study and provided; the concept and design, interpretation of the data, drafting of the manuscript, final approval to be published. SJM managed patient information, data analysis and final revisions of manuscript. SKS managed patient outreach and data collection. CMS managed patient outreach and data collection. JFG provided concept and design, data analysis and interpretation, final revisions of manuscript.
Patients consent
Please note that written informed consent was obtained from the patient (signed consent 2007; DOD 8/23/2011) whose photo is shown in Figure 1 for publication of this manuscript. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
REferences
[1].ystrom L, Andersson I, Bjurstam N, et al: Long-term effects of mammography screening: updated overview of the Swedish randomized trials. Lancet 16: 359-310, 909-919, 2002[pubmed]
[2].arly Breast Cancer Trialists’ Collaborative Group (EBCTCG): Effects of chemotherapy and hormonal therapy for early breast cancer on recurrence and 15-year survival: an overview of the randomized trials. Lancet 365:1687-1717, 2005[pubmed]
[3].nternational Breast Cancer Study Group: Effectiveness of adjuvant chemotherapy in combination with Tamoxifen for node-positive postmenopausal breast cancer patients. Jour Clin Oncol. 15(4): 1385-1394, 1997[pubmed]
[4].itrin DL, Bloom DL, Grutsch JF, et al: Beliefs and perceptions of women with newly diagnosed breast cancer who refused conventional treatment in favor of alternative therapies. The Oncologist 17 (5): 607-612, 2012[pubmed]
[5].ichards MA, Westcombe AM, Love SB, et al: Influence of delay on survival in patients with breast cancer: a systematic review. Lancet 353: 1119- 1126, 1999[pubmed]
[6].aplan LS, Helzlsouer KJ, Shapiro S, et al: Reasons for Delay in Breast Cancer Diagnosis. Preventive medicine 25 issue 2: 218-224[pubmed]
[7].alker QJ, Gebski V, Langlands AO: The misuses of mammography in the management of breast cancer revisited. Med J Aust. 151: 509- 512, 1989[pubmed]
[8].fzelius P, Zedeler K, Sommer H, et al: Patient's and doctor's delay in primary breast cancer. Acta Oncol. 33: 345- 351, 1994 [pubmed]
[9]oensuu H, Asola R, Holli K, Kumpulainen E, Nikkanen V, Parvinen L-M: Delayed diagnosis and large size of breast cancer after a false negative mammogram. Eur J Cancer. 30A: 1299- 1302, 1994[pubmed]
[10]Coveny EC, Geraghty JG, O'Laoide R, et al: Reasons underlying negative mammography in patients with palpable breast cancer. Clin Radiol. 49: 123- 125,1994[pubmed]
[11].Burgess CC, Ramirez AJ. Richards MA, et al: Who and what influences delayed presentation in breast cancer? Br J Cancer. 77: 1343- 1348, 1998[pubmed]
[12]. Tartter PI, Pace D, Frost M, et al: Delay in the diagnosis of breast cancer. Ann Surg. 229: 91- 96, 1999 [pubmed]
[13].MacArthur C, Smith A: Delay in breast cancer and the nature of presenting symptoms. Lancet 1: 601-603, 1981[pubmed]
[14].Goodson WH, Moore DH: Causes of physician delay in the diagnosis of breast cancer Arch Intern Med. 162(12):1343-1348, 2002[pubmed]
[15].Osuch JR, Bonham VL: The timely diagnosis of breast cancer: principles of risk management for primary care providers and surgeons. Cancer 74: 271-278, 1994 (suppl 1)[pubmed][16].National Comprehensive Cancer Network (NCCN): NCCN guidelines for breast cancer patients (Accessed on May 16, 2012). www.nccn.org
[17].Klein S: Evaluation of palpable masses. Am Fam Physician 71: 1731-1738, 2005 (suppl 9)[pubmed]
[18].helan M, Dobbs J, David AS: ‘I thought it would go away’: patient denial in breast cancer. Journal of the Royal Society of Medicine 85: 206-207, 1992[pubmed]
[19].nderson BL, Cacioppo: Delay in seeking a cancer diagnosis: Delay stages and psychophysiological comparison processes. Brit Journal of Social Psychology 34: 33-52, 1995[pubmed]
[20].annin DR, Mathews HF, Mitchell J, et al: Influence of Socioeconomic and Cultural Factors on Racial Differences in Late-Stage Presentation of Breast Cancer. JAMA 279: 801-1807, 1998 (suppl 22)[pubmed]
[21].Sheinfeld Gorin S, Heck JE, Cheng B, et al: Delays in Breast Cancer Diagnosis and Treatment by Racial/Ethnic Group. Arch Intern Med 2006 (suppl 20); 166: 2244-2252, [pubmed]
[22].Hansen RP, Olesen F, Sorensen HT, et al: Socioeconomic patient characteristics predict delay in cancer diagnosis: a Danish cohort study. BMC Health Services Research 8: 49, 2008 [pubmed]
[23].Citrin DL, Grutsch JF, Mortensen SJ, et al: Lack of Patient Compliance with Adjuvant Therapy Guidelines is an Important Risk Factor for Recurrence in Early Breast Cancer. World J Psychosoc Oncol 2013; 2: 1-7 [Full text].

